What Is Heart Block? What Is AV Bundle? What Is Bundle Branch Block?
Heart block, AV bundle, or Bundle branch block is a disease of the electrical system of the heart, as opposed to coronary artery disease, which is a disease of the blood vessels of the heart. The heart of an individual with heart block beats irregularly and more slowly than normal. In some cases the heart may actually stop for up to 20 seconds, caused by a delay, obstruction or disruption along the pathway that electrical impulses travel through to make the heart beat.
Heart block may affect people who appear healthy. It is frequently a sign of some other underlying heart problem. Electrical impulses that make the heart beat may be slowed or blocked as a result of injury or damage to the heart muscle, or blockage of a blood vessel. Even alterations to impulses that last only a fraction of a second can cause bundle branch block (heart block).
Sometimes heart block can make it more difficult for the heart to pump blood properly through the circulatory system, meaning that muscles and organs, including the brain do not get enough oxygen to function properly.
Heart block itself does not usually require direct treatment. However, the underlying health conditions which generally accompany it, such as coronary heart disease, do.
Heart block typically causes lightheadedness, fainting (syncope) and palpitations. Coronary artery disease, on the other hand, causes chest pain (angina) or heart attack (myocardial infarction).
A healthy human heart beats at approximately 60 to 80 times per minute. A heartbeat is one contraction of the heart muscles, which push blood around the body. Every muscle contraction is controlled by electrical signals that travel between the atria (the upper chambers of the heart) and the ventricles (the lower chambers).
- Partial heart block - this is when the electrical impulses are delayed or stopped. The heart does not beat regularly.
- Complete heart block - this is when the electrical signals are completely stopped. The heartbeat will drop to about 40 times per minute.
- First degree heart block - generally refers to minor heartbeat disruptions, such as skipped beats. It is the least serious type of heart block and does not generally require treatment.
- Second degree heart block - some electrical signals never get to the heart, causing drooped beats. The patient commonly experiences dizziness and may need a pacemaker.

- Third degree or complete heart block - electrical signals do not travel between the atria (upper chambers of the heart) and ventricles (lower chambers of the heart). This type is more common in patients with heart disease. If not treated with a pacemaker there is a serious risk of heart attack.
What are the signs and symptoms of heart block?
A symptom is something the patient feels and reports, while a sign is something other people, such as the doctor detect. For example, pain may be a symptom while a rash may be a sign. The main signs and symptoms of heart block include:- Slow or irregular heartbeats
- Shortness of breath
- Irregular heartbeat is felt (palpitations)
- Lightheadedness
- Syncope (fainting)
- Presyncope - a feeling that you are about to faint
- Possible pain or discomfort in the chest
- Difficulty in doing exercise, because not enough blood is pumped around the body
What are the causes of heart block?
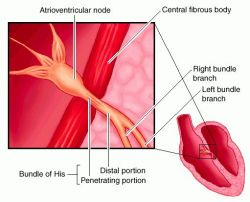
In a healthy heart electrical impulses that travel inside a heart muscle signal it to contract - to beat. The impulses move along a pathway; from the atria (upper heart chambers), through the AV (atrioventricular) node, to the ventricles (lower heart chambers).Along this pathway there is a cluster of cardiac fibers - the bundle of His - which divides into two branches; the right and left bundles. Each heart ventricle has a branch. If there is damage to one of these branch bundles the heart may not beat properly. The impulses that tell the heart to beat may be blocked or slowed down, resulting in uncoordinated ventricular contractions. The following may cause a bundle branch block:
- Cardiomyopathy
- Coronary thrombosis
- Myocarditis
- Valvular heart disease
- Post-operative development of scar tissue in the heart
Diagnosing heart block
A GP (general practitioner, primary care physician) will discuss symptoms with the patient and listen to his/her heart. Based on patients' signs and symptoms, age, as well as medical history, the GP may suspect heart disease. If so, the individual will be referred to a cardiologist (a doctor who specializes in heart conditions).The following diagnostic tests may be ordered:
- An ECG (electrocardiogram) - this is the most common test for detecting bundle branch block (heart block). The device records the patient's heart's activity. A technician placed probes on the skin of the chest which reveal the patterns of electric impulses through the heart as wave patterns. Certain wave abnormalities may indicate bundle branch block. This test can also determine which bundle branch is affected (the left or right).
- Holter tape - the patient wears a portable device which records all their heartbeats. It is worn under the clothing and records information about the electrical activity of the heart while the person goes about his/her normal activities for one or two days. It has a button which can be pressed if symptoms are felt - then the doctor can see what heart rhythms were present at that moment.
- Echocardiogram - this ultrasound scan allows the doctor to see the heart muscles and valves.
- Electrophysiology test - tiny electrical shocks are used to determine the cause of the abnormal rhythm (where in the heart).
- Tilt-table test - the patient is placed on a tilt table bed which changes his/her position. This test may sometimes provoke abnormal heartbeats (arrhythmia).
What are the treatment options for heart block?
There is no heart-block-specific treatment. The majority of people with bundle branch block are symptom free and do not require treatment. However, those with underlying conditions which may be causing the heart block will need to have treatment for the underlying condition.Because heart block affects the electrical activity of the heart, it may sometimes be more difficult to promptly diagnose other heart conditions, especially heart attacks.
Medication - these will be used to treat underlying conditions, such as hypertension (high blood pressure) or the effects of heart failure.
According to the American Heart Association, people with left bundle branch block who have had a heart attack should receive reperfusion, which is given in an emergency situation. Streptokinase, or a tissue plasminogen activator to dissolve blood clots and raise the flow of blood to the heart are administered. Both medications carry an elevated risk of bleeding.
A pacemaker - if the patient has a history of fainting, doctors may recommend implanting an artificial pacemaker. This is a battery-operated device which is implanted under the skin. It is about the size of a quarter (US coin) and weighs less than an ounce. They are placed near the patient's collarbone during a surgical procedure that lasts from one to two hours. The patient receives a local anesthetic.
Pacemakers today are extremely sophisticated; many can be set to produce an electrical impulse only when one is required. Some modern ones can tell if the heart stops beating and produce an electrical impulse to restart it. These devices can last many years before the generator (battery) needs to be changed.
Pacemakers are not affected by cell phones, personal stereos or household appliances. A person who has a pacemaker should not undergo an MRI (magnetic resonance imaging) scan.
What are the complication s of heart block?
s of heart block?
People with a left side bundle branch block have a higher risk of complications than those with a right side one. Examples of complications include: - Arrhythmia (irregular heart beat)
- Bradycardia (low heart rate)
- Cardiac arrest - there is either no contraction or inadequate contraction of the left ventricle of the heart, causing immediate, bodywide circulatory failure
- Sudden cardiac death - the unexpected death of an individual due to cardiac causes which occurred within 1 hour of symptom onset.

No comments:
Post a Comment